Myofascial pain syndrome is a long-term condition that causes pain in the muscles. The discomfort comes from pressure on sensitive areas or trigger points and is often the result of repetitive occupational activities or strain from physical exercise. Often, individuals feel pain in areas other than the affected muscles, which is known as referred pain.
Common Symptoms
People with myofascial pain syndrome (MPS) often experience an aching sensation deep within the muscle. The pain is likely to be long-lasting and usually worsens over time. Certain physical activities can also exacerbate pain. Sometimes, people with MPS feel firm, knotted areas around the affected muscles. The pain can interrupt normal day-to-day activities and prevent the person from getting adequate sleep.
Causes
Myofascial pain syndrome begins when trigger points develop within a muscle. These trigger points are sore patches where the muscle fibers are very tight, usually as the result of an injury, strain, or repetitive activity carried out over time. These trigger points become more and more painful as time passes. When the pain becomes chronic, doctors may diagnose myofascial pain syndrome.
Common Risk Factors
Some people are more at risk of developing trigger points in their muscles than others. People who continually put their muscles under intense stress are at a higher risk. Poor posture can also create trigger points, as can high levels of stress and anxiety manifesting as muscle tension. Over time, this tension can lead to tightening of the muscle fibers.
Diagnosis
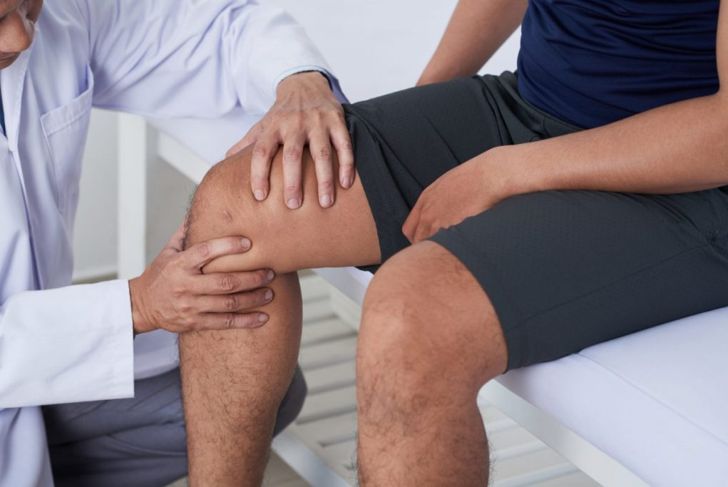
To diagnose myofascial pain syndrome, a doctor will carry out a physical exam of the affected areas. He or she will feel the muscles for areas that are particularly tight or painful and may apply pressure to any tender points. Responses to this pressure, such as involuntary muscle spasms, may indicate myofascial pain syndrome. If there is any doubt about the diagnosis, the doctor may order additional tests to rule out other common causes of muscular pain.
Medication for Myofascial Pain Syndrome
A doctor may recommend treating the pain caused by MPS with medication. Often, over-the-counter pain relievers can help, although the doctor may prescribe stronger medicines if the pain is severe. Some antidepressants effectively treat pain associated with the condition, and affected individuals may also require psychological treatment for secondary symptoms. People experiencing sleep disturbance as the result of their pain may take sedatives or sleeping pills.
Physical Therapy
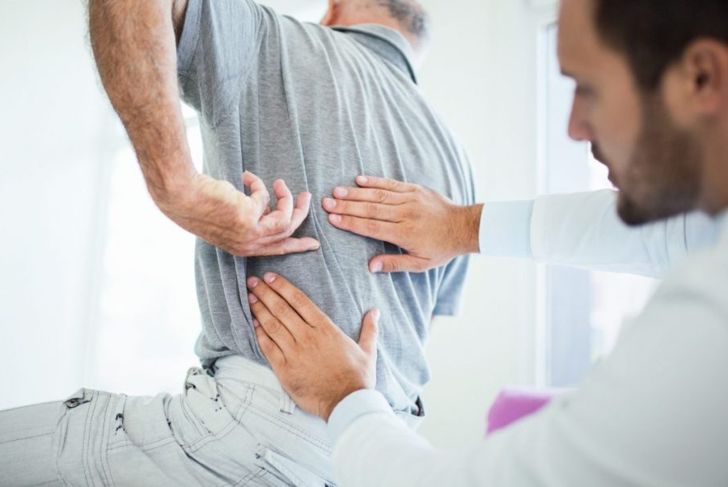
The doctor may recommend physical therapy in addition to or instead of medication. The therapist will prescribe particular stretches to reduce pain and tension in the muscles and improve posture, and may also use massage to help relax the muscle fibers. Applying heat packs to painful areas can provide additional relief.
Needle Therapy
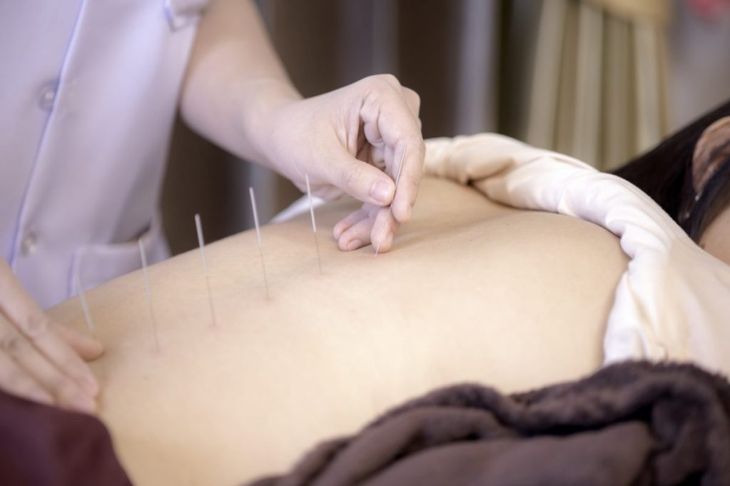
Several needle therapies may be helpful for myofascial pain syndrome. A doctor can inject local anesthetic or steroids into the painful area to relieve pain. Another option is dry needling: inserting a needle in various places around the trigger point. Studies show this practice can be an effective pain relief measure. There is also some evidence to show acupuncture helps people with MPS.
Home Remedies
In addition to therapies prescribed by a doctor, self-care methods can help people with myofascial pain syndrome ease or control their symptoms. Gentle exercise can help ease muscle tension. Taking steps toward managing stress will reduce muscle pain caused by clenched muscles.
Complications
Research suggests some people with myofascial pain syndrome may eventually develop fibromyalgia, a chronic condition that causes pain across the body. Experts believe the condition develops as people become more sensitive to pain signals over time, a primary symptom of fibromyalgia.
When to Seek Help
Many people with myofascial pain syndrome delay seeking medical help because they believe experiencing muscle pain is normal. While it is true that everybody experiences muscle pain at some point, pain that is persistent or gets progressively worse requires evaluation by a doctor. Usually, muscle pain will improve with simple self-care measures such as rest and stretching. If nothing eases the pain, this is another sign one needs to see a doctor.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More