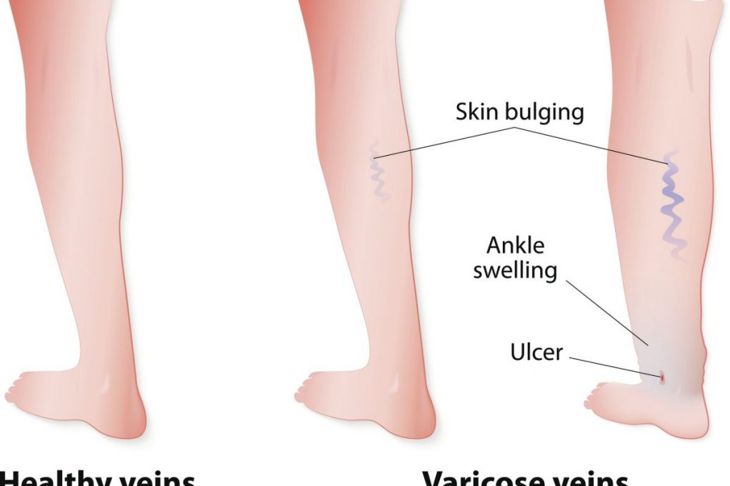
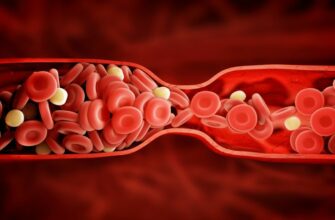
Thrombophlebitis, commonly known as phlebitis, is an inflammatory condition of a vein, generally in the leg, though in rare instances the condition can develop in the arms and neck as well. The primary symptoms of thrombophlebitis are redness and swelling in a specific area that may feel warm to the touch. In many cases, phlebitis is not a serious health issue; it is common among individuals with varicose veins. However, if a clot causes the inflammation in the vein, phlebitis can escalate in severity and danger.
Types of Phlebitis
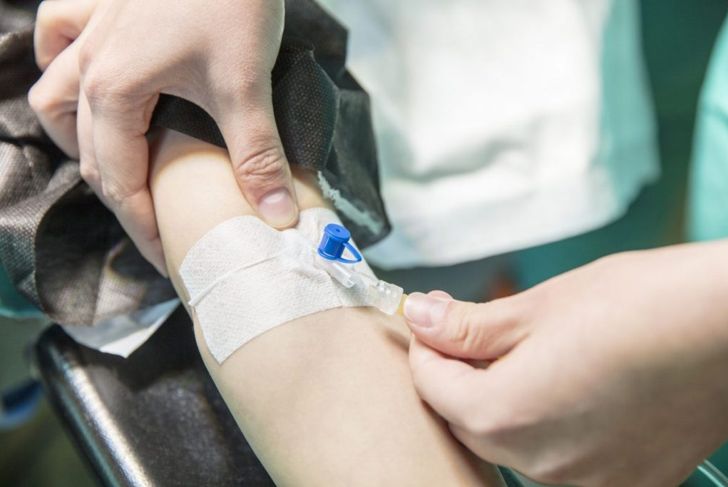
There are two types of phlebitis: superficial and deep. Superficial phlebitis occurs in a vein just beneath the surface of the skin and is often the result of mild trauma to the vein, such as that caused by an IV catheter. It may appear as a red, hardened, twisted cord under the surface of the skin. Deep phlebitis occurs within a vein hidden in a muscle and is generally associated with a blood clot that blocks the vein. It cannot be detected visually. With both types, more than one vein may be affected.
Symptoms of Superficial Phlebitis
The most noticeable sign of superficial phlebitis is a series of hard, painful lumps underneath the skin. There may be a red streak on the skin’s surface, accompanied by swelling and tenderness in the area, or the skin over the vein may turn dark. The red, itchy patch may feel warm and tender, and the individual may have a low-grade fever. Superficial phlebitis can also occur around the site of an irritating IV.
Symptoms of Deep Phlebitis
When it affects a larger, deeper vein and a blood clot forms, the doctor may diagnose the patient with deep vein thrombosis (DVT). There are no visible symptoms because muscle covers the veins. Only half of the people with DVT show any symptoms at all until serious complications develop. Pain may occur in the calf or thigh and may be more noticeable in the foot while walking or flexing. DVT is a more serious issue than superficial phlebitis because a blood clot could break loose and travel through the bloodstream to the lungs.
Causes of Superficial Phlebitis
Immobility is a primary cause of phlebitis, especially when one is confined for a long period, such as patients in a hospital with limited physical activity. An individual who has varicose veins, is pregnant, or is recovering from pregnancy is more likely to develop it. The condition can also occur around IV sites, or as a result of receiving medications intravenously. In some cases, because of an infection. Obesity, smoking, age, and oral contraceptives may also contribute.
Causes of Deep Phlebitis or a DVT
Certain medical conditions are associated with DVT, such as connective tissue and genetic blood clotting disorders. People who had DVT previously have a higher probability of recurrence. Trauma resulting from surgery, a broken bone, or a serious injury can also cause a DVT. Often, bedridden individuals develop DVT due to lack of physical movement and the resulting slower blood flow. Some cancers and their treatments are linked to DVT, as is hormone replacement therapy.
Venous Thromboembolism
Venous thromboembolism is a serious vascular disease that also starts in the vein, and DVT and pulmonary embolisms are forms of the condition. With long periods of non-movement, blood flow in the legs slows and pools, and blood clots may form. If those clots break off, they travel through the bloodstream to the lungs, where they can cause a pulmonary embolism (PE). Some symptoms of PE include chest pain, coughing, irregular heartbeat, and shortness of breath, but there are minimal, if any, symptoms for DVT.
Diagnosing Phlebitis
Doctors can usually diagnose phlebitis through a physical exam and may order tests such as an ultrasound, which will show the blood flow through the affected area and reveal the location of a clot. The physician may also use an evaluation called a D-dimer level assessment, which requires drawing blood and checking for the presence of D-dimer, a protein released into the bloodstream when a blood clot dissolves. A positive D-dimer test usually results in additional testing such as MRIs, venography, or CT scans.
Prevention
People who have a higher risk of phlebitis include those who are overweight or over the age of 60, as well as smokers, people who consume excess alcohol, and people who have had a stroke. Eating a healthy diet and losing weight can help prevent phlebitis. Increasing activity and reducing the amount of time spent sitting or laying down can also reduce risk. People taking birth control pills or undergoing hormone therapy should be aware that blood clots are a side effect and can cause phlebitis or DVT.
Treatment
Swelling, tenderness, redness, or pain in the legs are warning signs, especially if an individual has a history of stroke, DVT, or phlebitis. Generally, superficial phlebitis is treated at home. The doctor will recommend support stockings, warm compresses, and anti-inflammatory over-the-counter drugs. However, DVT is much more serious, and unfortunately, the first symptoms often do not occur until after complications begin to develop. Most people take blood thinners, and in some cases, a filter device is inserted into the inferior vena cava, which carries blood from the body back to the heart, to further reduce clotting.
Prognosis
Superficial phlebitis usually clears up within a week or two. If the issue results in a hardening of the vein or an infection, recovery may take a bit longer. Varicose veins indicate a likelihood that phlebitis will return. DVT always requires medical treatment and follow-up. If an individual had DVT before, chances are it will occur again. Those who seek medical attention at the first sign of swelling, redness, or pain in the legs, have a better chance of avoiding more serious complications.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More