Fallen arches occur when the arch of the foot goes flat or collapses entirely. Because this has such a significant impact on standing and walking, people with fallen arches can experience pain that is at times debilitating. Various interventions can ease the effects of fallen arches, including orthotics and surgery. Fallen arches are relatively common and can affect any adult. Interventions are more effective if the condition is caught early.
Adult-Acquired Flatfoot
Fallen arches are also referred to as adult-acquired flatfoot. This is a much different condition than pediatric flatfoot, a condition some children are born with that often resolves on its own. Fallen arches are a common condition of the ankles and feet that can affect both men and women. When fallen arches occur in adulthood, the condition is permanent and can worsen over time.
Risk Factors
Anyone can develop fallen arches, but they most commonly affect females over the age of 40. Pregnant women are also at higher risk, as are people of both genders with obesity, hypertension, diabetes, and rheumatoid arthritis. Those who also had flat feet as children are more likely to develop fallen arches in adulthood.
Posterior Tibial Tendon Dysfunction
There isn’t a singular cause of fallen arches, but one of the most common is posterior tibial tendon dysfunction or PTTD. The posterior tibial tendon supports the arch of the foot and runs down the inside of the lower leg from the calf to the inner foot. Fallen arches can occur when this tendon is injured, torn, or overused. It is a common cause of fallen arches in women and athletes who play sports like soccer or basketball.
Lisfranc Injury
A Lisfranc injury occurs if bones in the middle of the foot break or the ligaments that support the midfoot tear. This severe injury can also damage the cartilage in the foot. The arch of the affected foot can collapse if the injury is not treated surgically. A Lisfranc injury can be the result of a simple twist and fall and is commonly seen in soccer players but can also occur from a simple stumble. Injuries to the back of the foot or within the foot can cause fallen arches, too.
Charcot Foot
People with diabetes or peripheral neuropathy can develop Charcot foot. These conditions decrease sensitivity in the feet, which means the person may not notice an injury right away. This can lead to more severe deformities before a doctor can make an official diagnosis. The bones in the foot weaken, and the arch eventually collapses. Other bones in the foot may break as well.
Symptoms of Fallen Arches
Symptoms of fallen arches vary depending on the cause. If PTTD is the cause, the person may feel pain from the inside of the foot up toward the calf and may experience swelling in the ankle. People with diabetes may not notice anything at first but will eventually see swelling or notice skin sores on the bottom of the feet that do not heal easily.
Other Symptoms of Fallen Arches
Some more general symptoms of fallen arches include foot pain when walking or standing that gets worse after a vigorous activity such as power walking or jogging. Collapsed arches put more pressure on the ankle, so ankle pain develop as well. Finally, bony bumps that appear on the inside or top of the foot can signal fallen arches due to changes in the structure and anatomy of the foot.
Diagnosis
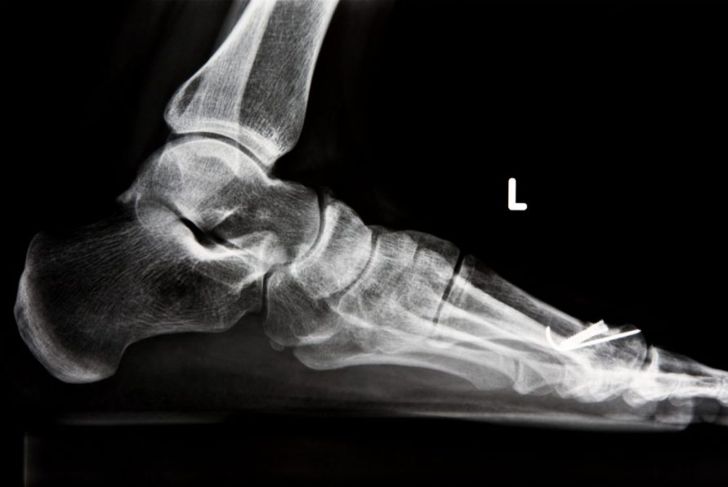
Diagnosis of fallen arches begins with a visit to a doctor, who will examine the mechanics of the feet. If the person is experiencing a lot of pain, the doctor may order imagining tests. X-rays can pick up on deformities and arthritis, and CT scans can provide views from different angles. An MRI can give details of any soft tissue damage, and ultrasound is useful for evaluating injured tendons.
Treatment
There are a few ways to treat fallen arches. None of them can repair the actual damage, but they can alleviate pain and make the person more comfortable. Over-the-counter arch supports may help provide additional support, though some people require custom-made orthotics. Supportive athletic shoes are often more comfortable than flat sandals or slip-on shoes.
Physical Therapy
Stretches can also be beneficial for people with fallen arches, particularly if they also have a shortened Achilles tendon. Another option is physical therapy. Sometimes fallen arches can cause damage to other joints due to change in gait. A physical therapist can analyze how the person walks and runs to help modify their technique to cause less pain.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More