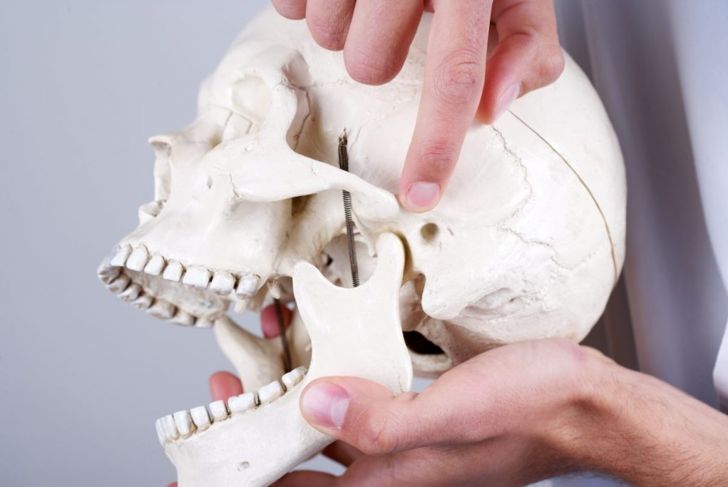
The temporomandibular joint (TMJ) works like a sliding hinge connecting each side of the jaw bone to the temporal bones of the skull. The bones and joint are separated by cartilage and shock-absorbing disks to help the jaw open and close smoothly. One joint sits on each side of the jaw, and if one of these joints or the muscles around them develop problems, one or both joints can develop temporomandibular joint dysfunction. TMJ dysfunction causes pain in the jaw, joint, or temporal bone areas of the skull.
Cause
Doctors and dentists are unsure exactly what causes TMJ dysfunction, and the cause appears to vary from person to person depending on their habits and medical background. TMJ dysfunction may occur if the shock-absorbing disk erodes partially or completely or moves out of proper alignment. People with arthritis may experience painful TMJ dysfunction due to cartilage damage. An injury to the joint or surrounding area from impact can also lead to TMJ dysfunction.
Risk Factors
People with rheumatoid arthritis and osteoarthritis are more likely to develop TMJ dysfunction. Connective tissue diseases can also elevate risk, as can jaw injuries or injuries to the surrounding bone, even if the immediate area affected does not seem linked to the temporomandibular joints. Long-term teeth grinding or clenching can also be a significant risk factor, and those with more stress in their lives are more likely to develop TMJ dysfunction since stress often leads to clenching and grinding.
Symptoms
Symptoms can range from a dull ache to intense, sharp pain. The most common symptom of TMJ dysfunction is pain or tenderness in the face, jaw joint, and even the neck, shoulders, or around the ear while talking, speaking, chewing, or just opening or closing the mouth. Some people experience problems when opening the mouth wide — the jaw may lock either open or closed. Clicking, popping, and grating sounds when opening and closing the mouth, trouble chewing, and swelling on the side of the face can occur, as well.
Diagnosis
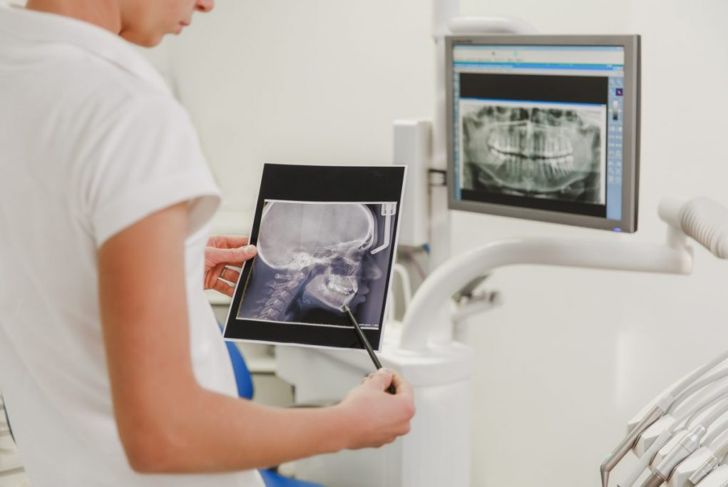
Other conditions affecting the teeth and sinus problems can cause symptoms similar to those of TMJ dysfunction, so it is important to receive an accurate diagnosis from a doctor or dentist. Most doctors will check the jaw for pain or tenderness and abnormal noises when opening and closing. They may also check the bite of the jaw and the facial muscles. The doctor may take full-face x-rays to better examine the jaw, joint, and teeth and may also order an MRI or CT.
Treatment: What to do
For most cases, doctors recommend at-home treatment for TMJ dysfunction. Resting a hot or cold pack on the jaw for about ten minutes a few times a day at a time can help ease pain and relax tension. Eating soft foods reduces the need to chew or bite down hard, and cutting tougher foods into smaller pieces prevents the need for the jaw to open wide. Short-term use of anti-inflammatory drugs can relieve pain and swelling as well. Reducing stress and addressing teeth clenching or grinding with a mouthguard or other method will also help relax the jaw.
Treatment: What to avoid
People with TMJ dysfunction should strive to avoid extreme jaw movements such as large yawns or big bites. It is best to avoid resting the chin in the hand or putting the head and jaw into strange positions. They should keep away from tough, hard, or chewy foods, and most doctors recommend avoiding dental procedures that permanently change the bite or jaw such as crowns, bridgework, or splints. For some patients, however, these changes are required to address the cause of TMJ dysfunction.
Treatment: Exercises
Jaw exercises can help relieve TMJ pain by relaxing, stretching, and strengthening the jaw. Doctors will recommend the best exercises based on cause and symptoms. These include relaxing the jaw by gently placing the tongue on the roof of the mouth, repeated chin tucks, and forward and side-to-side jaw movement.
More Treatments for TMJ Dysfunction
If home treatments and exercises prove ineffective, dentists may recommend transcutaneous electrical nerve stimulation (TENS). This procedure uses low-level electrical currents to relax the jaw and surrounding facial muscles. Ultrasounds apply heat and relax the joint, and radio wave therapy stimulates the joint, increasing blood flow to the jaw and decreasing pain. Acupuncture, massage, and chiropractic care can all treat TMJ problems as well.
Surgery for Temporomandibular Joint Dysfunction
Surgery is usually not necessary, and many experts recommend avoiding surgery and permanent changes to the jaw if possible. However, sometimes TMJ dysfunction becomes severe enough that it requires surgery, and physicians turn to three types. Arthrocentesis is a minor procedure common for those with a locked jaw but no history of TMJ dysfunction. Arthroscopy lets the doctors see inside the joint and remove inflamed tissue or realign the joint. The minimally invasive procedure usually leaves only a small scar. Open-joint surgery is more invasive and requires a longer recovery time, but may be necessary in certain, serious cases.
Long-term Outlook
In most cases, self-care and simple treatments will help alleviate TMJ dysfunction successfully. Some people experience the symptoms off and on over the years, with pain usually fading within a few days to weeks, but if doctors can address the cause, TMJ is much less likely to be a reoccurring problem.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More