Gangrene is the death of body tissue due to a lack of blood supply and is most often seen in the extremities, internal organs, or muscles. People with diabetes or atherosclerosis (hardened arteries) are at the highest risk of developing gangrene. There are many types of gangrene, but they tend to share similar treatments. Doctors typically treat the condition by removing dead tissue, using hyperbaric oxygen therapy, or antibiotics. If caught early, medical care can heal gangrene, and affected body parts do not necessarily require amputation.
Symptoms
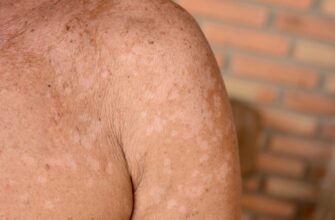
Skin discoloration is one of the first signs of gangrene. The skin may become pale, black, purple, fiery red. The type of gangrene often determines the color, Gangrenous skin also swells, sometimes forming blisters, and looks damaged. Individuals with the condition may notice skin in a certain area is thinner than the rest and hair growth stops. Often, the skin is cool to the touch and may exude a discharge with a foul smell. When gangrene is advanced, individuals experience numbness or develop a low-grade fever, especially if the gangrene has damaged tissue beneath the skin. If a bacterial infection is responsible for the condition and begins to spread, it is possible to develop septic shock. People who have this kind of gangrene may have a rapid heartbeat, shortness of breath, and feel confused.
Causes
Although many people associate gangrene exclusively with diabetes, several factors can cause this condition. Any event that cuts off blood and oxygen supply to organs or tissues elevates the risk of gangrene. The nutrients in blood and oxygen feed the body’s cells and boost the immune system to fight infection. After being cut off from blood and oxygen for a time, the tissues start to decay. This can also happen following trauma such as a gunshot wound or other injury. The bacteria that form after an injury can invade damaged tissue and cause gangrene. The same is true with a bacterial infection, especially if the individual is unaware that it exists. The infection eventually kills the tissue and leads to gangrene, if untreated.
Wet Gangrene
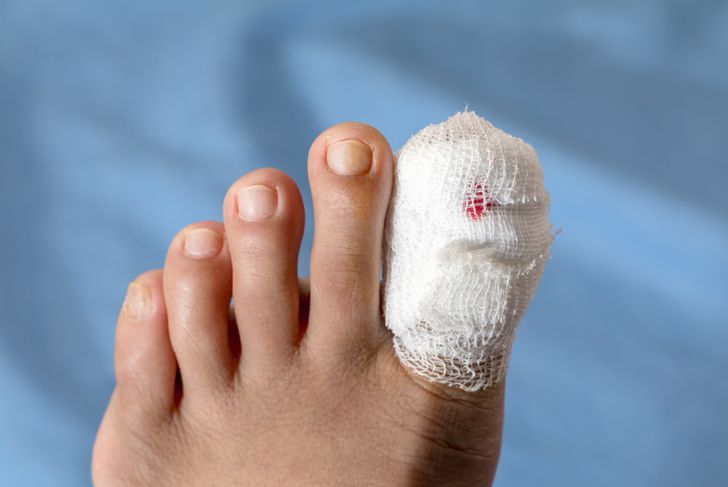
Wet gangrene occurs when a bacterial infection in the affected tissue creates a wet appearance. This type of infection includes swelling and blistering. Some people develop wet gangrene after an injury, or after experiencing frostbite or a severe burn. This form of gangrene is noticeable in people who have diabetes and who unknowingly injure their toes or feet. It spreads quickly and can be life-threatening if not immediately addressed by a doctor.
Dry Gangrene
Dry gangrene presents with dry, shriveled areas on the surface of the skin. It develops slowly and can appear in a range of colors, including brown, black, blue, or purple. Medical experts note dry gangrene occurs most often in people with arterial blood vessel diseases. These people do not have enough oxygen going to organs like the heart, muscles, and liver. Over time, the part of the body getting too little oxygen will start to deteriorate. Because the skin remains closed over the deteriorating tissue, dry gangrene is less noticeable.
Gas Gangrene
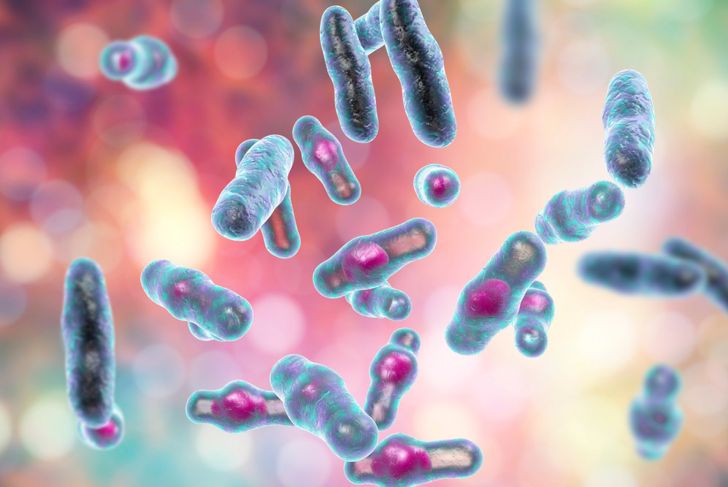
Like dry gangrene, people with gas gangrene may not notice at first, as the skin can remain unblemished. This version of gangrene causes gas to develop in deep muscle tissue. Over time, the skin will begin to change color and may appear bubbly and make a crackling sound when you press on it. The most common cause of gas gangrene is the Clostridium perfringens bacterium, which tends to be contracted through surgical wounds. Toxins from the bacteria release gas, destroy tissue, and can lead to death.
Internal Gangrene
If the body does not receive enough oxygen, gangrene can develop in the organs. The gallbladder and appendix can be affected by internal gangrene, as can other organs. People with internal gangrene experience severe pain and fever, and the condition can be fatal.
Fournier’s Gangrene
Gangrene can affect the genital areas of your body. In the case of Fournier’s gangrene, an infection in the genitals or urinary tract prompts tenderness, redness, pain, and swelling. Fournier’s occurs more often in men than in women. It was first identified in 1883 by French venereologist Jean Alfred Fournier, who treated five young men experiencing rapidly progressing gangrene of the penis and scrotum.
Meleney’s Gangrene
Although surgery is often a life-saving measure, it can also result in infection. If painful skin lesions develop up to a couple of weeks after surgery, it is possible the former patient has developed a rare condition known as Meleney’s gangrene. This occurs most often after thoracic and abdominal procedures and develops from a mix of bacterial infections, including Staphylococcus aureas. Pain is the most significant symptom of this kind of gangrene, and it does not generally lead to wide-spread toxicity.
Risk Factors
Diabetes is one of the most common risk factors for developing gangrene. High blood sugar can damage blood vessels and disrupt blood flow to the body. Other conditions that increase one’s risk include injuries, surgery, blood vessel disease, and medications or drugs that cause bacterial infections. Two factors within our control can also lead to gangrene: smoking and obesity; the latter adds extra weight that compresses arteries. People suppressed immune systems are also at a higher risk.
Prevention of Gangrene
Some self-care measures will reduce the risk of developing gangrene. People with diabetes should watch for cuts, sores, and infection, and control their blood sugar. Other preventive measures include avoiding tobacco products and maintaining a healthy weight. It is also helpful for people who are at risk for gangrene to keep a close watch on their skin during cold weather. Frostbite, which leaves the skin cold, numb, pale, and hard, can lead to gangrene.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More