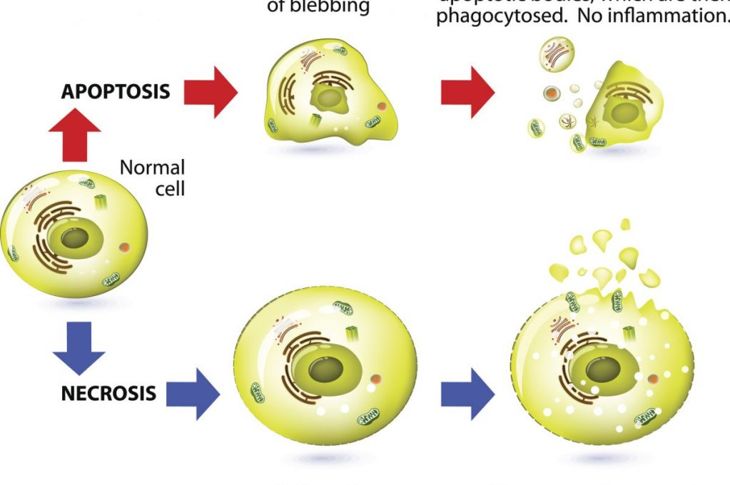
Sometimes called “second cell death,” necrosis is the opposite of apoptosis or programmed cell death. During necrosis, tissue dies without anything to trigger the next step: phagocytes that clean up and recycle the dead cells. Instead, the debris accumulates and causes inflammation, spurring a cascade of events. Chemicals released in necrosis start a chain reaction that damages other systems. Necrosis generally requires prompt medical treatment to avoid serious consequences.
Causes of Necrosis
The causes of necrosis can be internal or external. External circumstances include injury to the body that causes cell damage or destruction, or ischemia, a disruption of blood supply to tissues. An example is frostbite: ice crystals put pressure on cells, causing them to burst. Internal factors include bacteria, toxins, and damaged or defected nerve cells. The venom from the Asian giant hornet, Vespa mandarinia, and recluse spiders from the U.S. and South America impart toxins that can cause necrosis.
Coagulative Necrosis
Under normal circumstances, dealing with dead cells involves enzymes that break down proteins into recyclable amino acids. When coagulative necrosis occurs, something alters the natural qualities of these proteins. Albumin, for example, becomes a firm and opaque gel that remains in dead tissues. This type of necrosis is usually caused by severe ischemia in tissues of the adrenal glands, kidney or heart. In most cases, labile cells — cells that constantly multiply — replace dead cells. The exceptions are neurons and cardiomyocytes, which the body cannot replace once lost.
Liquefactive Necrosis
Liquefactive necrosis or colliquative necrosis can occur following bacterial or fungal infections, or chemical burns. Dead cells that have been digested by hydrolytic enzymes — those that use water to separate larger molecules into parts — become a viscous liquid mass. This necrotic pus can form abscesses, particularly in the brain, which is rich in waste-disposal enzymes called lysosomes.
Fat Necrosis
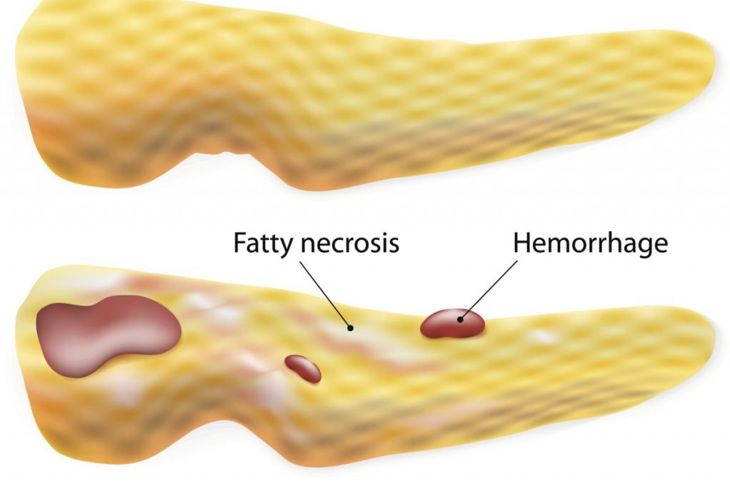
When the enzyme lipase releases fatty acids from triglycerides, it binds with calcium and appears as chalky white clumps — fat necrosis. Though it’s associated with trauma of the pancreas or acute pancreatitis (sudden inflammation of the pancreas), it may also occur in the breast as a pseudo-mass or lump. Fat necrosis in the breasts is almost always an after-effect of breast surgery or radiation.
Fibrinoid Necrosis
Fibrinoid necrosis happens when an accumulated protein-like substance that looks like fibrin — white insoluble fibrous protein — leaks and combines with the antigen and antibodies in the walls of blood vessels. If the debris is not destroyed or reabsorbed, it attracts calcium salts and other minerals and becomes calcified. Malignant hypertension, preeclampsia, and immune reactions such as hyperacute transplant rejection are common causes of this type of necrosis.
Caseous Necrosis
This type of necrosis happens when dead cells don’t digest completely. It’s a combination of liquefactive and coagulative necrosis from fungi, mycobacteria that cause illnesses such as tuberculosis and leprosy, or foreign objects such as sutures. The cells take on a clumped-cheese appearance and leave behind granular particles. Caseous necrosis is comparable to a granuloma, which walls off substances it can’t eliminate and forms an inflammatory border in the process.
Gangrenous Necrosis
Gangrenous necrosis is a type of coagulative necrosis that looks like mummified tissue. It usually manifests in the lower limbs or gastrointestinal tract. Those with diabetes and peripheral artery disease have an increased risk of the disease. Dead tissue that becomes infected and causes liquefaction is wet gangrene. Symptoms include red or black skin that’s cool to the touch due to lack of blood supply, pain, and swelling. More serious symptoms include fever and sepsis, which, if left untreated, cause death.
Hemorrhagic and Gummatous Necrosis
Gummatous necrosis presents as coagulative and caseous. Gummas are soft growths, a type of granuloma. They occur during the third stage of syphilis due to the tissues’ reaction to the bacteria. These masses can develop all over the body, including in the brain, liver, and skin. Hemorrhagic necrosis occurs when deoxygenated blood cannot leave an organ; this interrupts tissue oxygenation and leads to tissue death.
Avascular Necrosis
Avascular necrosis or bone infarction is the death of bone tissue. While a clear cause is lacking in some cases, risk factors include excessive alcohol consumption, use of high-dose steroids, and bone fractures. When a factor reduces or removes blood supply, complete bone tissue death happens within a week, with the bone marrow fat cells being the last to go. Under favorable conditions, restoration of blood flow can prompt repair, resulting in new and functional bone tissue.
Treatments
The rule of thumb for dealing with necrosis is to treat the underlying cause of the disease — this will improve the prognosis. Antioxidants help counteract damage to membranes and proteins and debridement, surgical or non-surgical tissue removal, is a standard treatment. There are times when more radical treatments are necessary. Maggot therapy, specifically Lucilia sericata, is such an option. Maggots consume necrotic tissue and infection, stimulating the healing process. Additionally, studies show hyperbaric oxygen treatment is effective against some forms. In the most severe cases, patients may require complete removal of the limb or organ.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More