Hemifacial spasm is a neuromuscular disorder that causes involuntary spasms of the muscles on one side of the face. The spasms or tics usually occur on the left side and can last throughout the day and even during sleep. Hemifacial spasm affects approximately 11 out of every 100,000 people. Men and women can develop the condition, but women middle-aged and older are twice as likely to get hemifacial spasms. People of Asian descent have a slightly higher risk, as well.
Symptoms
The first symptom of hemifacial spasm is usually twitching in the muscles of the left eyelid. Spasms can be strong enough to cause tears and to force the eye to close. The spasms are usually isolated to only one side of the face, but some people develop them symmetrically. People usually start to develop symptoms of hemifacial spasm between the ages of 40 and 50.
Long-Term Effects
Untreated hemifacial spasms increase in severity and spread to affect more facial muscles. Larger spasms can involve muscles extending from the eye to the chin. When the tics affect the mouth muscles, they can pull the mouth to one side. All the muscles on the affected side of the face can eventually form a permanent frown. Other symptoms include clicking sounds in the ear, changes in hearing, and hearing loss.
Causes of Hemifacial Spasms
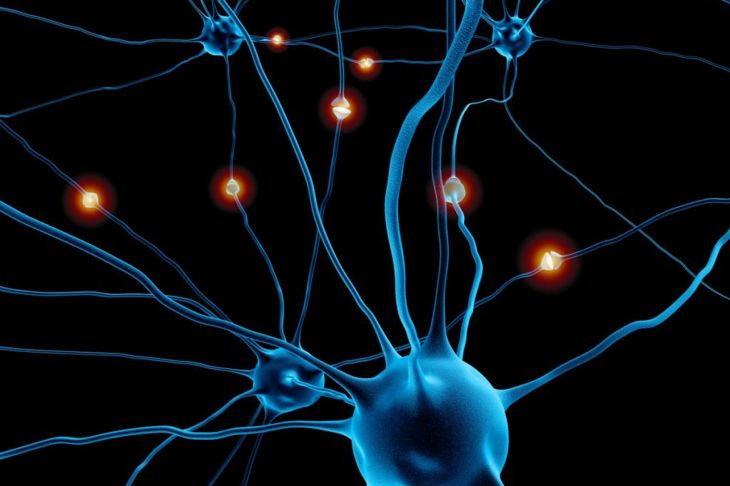
An irritated facial nerve is the most common cause of hemifacial spasm. This group of cells is the seventh cranial nerve and controls the muscles of the face. The facial nerve also transmits taste from the tongue and sensations in the ear. A small artery pressing on the facial nerve near the brain stem is usually the cause of irritation. Less common causes are nerve injuries, lesions or benign tumors putting pressure on the nerve, or abnormal blood vessel clusters at birth. Hemifacial spasms can be hereditary, but this is very uncommon.
Aggravating Factors
Hemifacial spasms are involuntary, so physical actions cannot prevent them, though medications can help. Stress, fatigue, and anxiety increase the severity and frequency of spasms and other involuntary tics not related to an underlying medical condition. As such, exercise, a well-balanced diet, stress-management techniques, and sufficient sleep help mitigate hemifacial spasm events.
Underlying Mechanism
Three theories explain how hemifacial spasms might occur. The ephaptic transmission theory states that arteries or other obstructions pushing the facial nerve out of place result in electrical activity between neurons, creating synapses where they should not exist. A second theory proposes that compression of the facial nerve causes abnormal activity in axons and dendrites at the base of the nerve. The kindling theory attributes facials spasms, hearing loss, and odd smells or tastes to “scrambled” feedback in the facial nerve following injury or compression.
Importance of Seeking Medical Help
It is important to see a doctor when one first notices signs of a hemifacial spasm, so evaluation and treatment can start early. In some instances, the spasms are an early symptom of multiple sclerosis, a disorder caused by the immune system attacking the central nervous system. MS is only the cause in one to six cases out of several hundred hemifacial spasm assessments. Doctors usually check for other signs of MS when a person under 40 presents with hemifacial spasm symptoms.
Diagnosis of Hemifacial Spasm
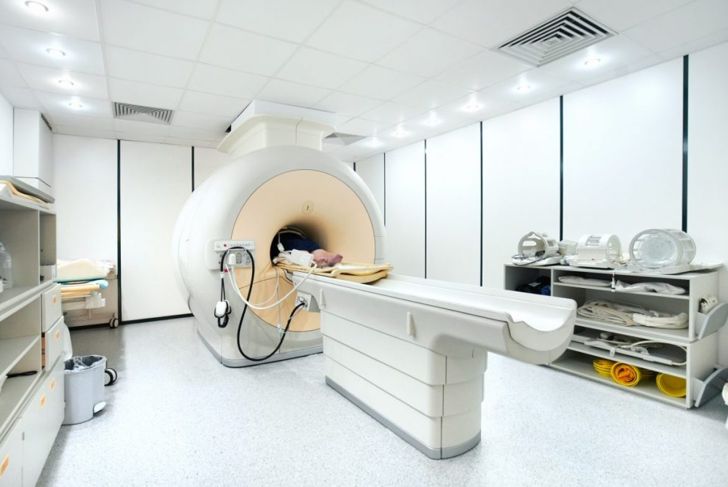
Doctors diagnose hemifacial spasm through physical examination, medical history, and imaging tests such as MRI or CT scans and angiography. Magnetic resonance imaging or MRI creates a detailed image with powerful magnets and radio waves. Sometimes doctors inject a contrast dye into a blood vessel to highlight abnormal blood vessels that could be irritating facial nerves. A magnetic resonance angiogram is an MRI scan that uses this dye.
Diagnostic Complications
Hemifacial spasms mimic symptoms of other disorders, such as Bell’s Palsy. The blood vessels surrounding the seventh cranial nerve are too small to see clearly with imaging tests. Doctors use diagnostic tests and symptom history to rule out other disorders, then search for the cause. When no other cause is evident, the condition is diagnosed as an artery compressing the seventh cranial nerve.
Treatment Options
Injections of botulinum toxin into affected muscles are effective for relieving hemifacial spasm symptoms 85 to 95% of the time. The paralysis the toxin causes provides immediate relief but is only temporarily, so follow-up treatment is required every three to six months. Anti-convulsant drugs are an alternative treatment option. Surgical intervention is a one-time procedure instead of a continuous process, but toxin injections and medications are less invasive.
Microvascular Decompression
Microvascular decompression is a surgical procedure that creates an opening in the skull and dura, the covering of the brain, to expose the facial nerve. The surgeon follows the seventh cranial nerve to its source in the brain stem and pushes the problematic artery away from the nerve. The surgeon then inserts a pad over the facial nerve to shield it from future compression and irritation. This procedure is effective approximately 85% of the time.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More