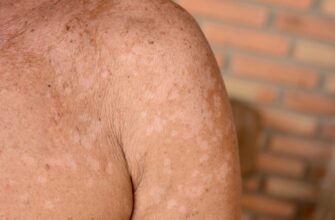
Lupus is a chronic autoimmune disease that leads the immune system to recognize healthy tissue as a threat and attack it in the way it would attack bacteria or viruses. Lupus can affect the skin, joints, and organs and has no cure. As such, treatment focuses on managing symptoms, which usually depends on what part of the body the disease affects the most and the severity of symptoms. Lupus may go into remission from time to time, but individuals often have lifelong flare-ups. Researchers continue to search for more information about the causes of lupus.
Gender
Because 90% of individuals with lupus are female, researchers have analyzed genetic differences between men and women. However, they have yet to find a link between lupus and female genetics. Research continues, however, and scientists are getting closer every day to determining the link.
Estrogen
Many studies delve into the link between estrogen levels and lupus. With the majority of those with lupus being women, estrogen may seem like the obvious link. Studies follow women with lupus using estrogen for birth control or menopause symptoms; thus far, an increase in estrogen has not been shown to affect lupus symptoms.
Ethnicity
Individuals from certain ethnic backgrounds are more prone to developing lupus. While the disease could relate to ethnic genetic factors, the studies have yet to prove or disprove this definitively. Individuals more prone to developing lupus are those of African, Asian, Hispanic or Latino, Native American, Native Hawaiian, or Pacific Island descent.
Genetics
Many individuals with lupus have family members who also have the disease. While there is likely a link between familial genetics and lupus, it is possible to develop lupus even if there is no family history. It is likely that there is an association between genetics and lupus. However, scientists have yet to discover exactly what that link is.
Chance
Unfortunately, in some cases, people with lupus appear to have the disease for no known reason. Often they have no family history or outside factors that appear to have contributed to the development of the disease. Although many ideas exist about why some individuals develop lupus, some people don’t appear to fit any of them.
Physical or Emotional Stress
Although it is not necessarily the exact cause, physical or emotional stress may contribute to lupus flare-ups. Emotional stress levels are often high during major life changes and events like changing jobs or a death in the family. Physical stress includes injury, surgery, or other illnesses or symptoms that use the body’s energy stores to heal.
Antibiotics
Some antibiotics have a tendency to induce lupus flare-ups. For example, antibiotics in the penicillin family can worsen lupus symptoms. In some individuals, taking a course of antibiotics triggers their first lupus flare-up, causing doctors to mistake lupus for allergic reactions or other conditions.
Exhaustion
Those with lupus must be careful not to overexert themselves, as lupus symptoms are known to worsen with overactivity or fatigue. Because of this, individuals who have lupus should always get adequate rest and downtime, as well as limit exercise, work, travel, and other activities that may result in fatigue.
Infection
When infection occurs, the immune system responds by attacking the virus or bacteria that is causing it. When a person has lupus, their body is unable to determine the difference between bad and healthy tissues. Therefore, when the immune system is fighting infection, it also increases its attack on healthy tissues.
Ultraviolet Light
Exposure to ultraviolet rays from sunlight, fluorescent light, or tanning beds can exacerbate symptoms of lupus. Those with lupus often complain of flare-ups occurring immediately after spending time outside in the sunshine. Exposure to sunlight can cause people with lupus to develop a skin rash, and medications that increase sensitivity to sunlight as a side effect may also have an effect on lupus flare-ups.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More