Nerve damage caused by diabetes is called diabetic neuropathy. Nearly half of all people with diabetes have some form of nerve damage. Neuropathy is most common in people who have had the condition for a long time. This nerve damage can lead to many issues. There are four main types of diabetic neuropathy, and an individual can have one or more at any time. Symptoms depend on the kind of neuropathy you have and which nerves are affected. Most cases of neuropathy develop progressively; you may not notice anything is wrong until considerable nerve damage has occurred.
Peripheral Neuropathy
Peripheral neuropathy is the most common type of diabetic neuropathy. This version initially affects the feet and legs, then spreads to the hands and arms. Symptoms are usually worse at night and include numbness or reduced ability to feel pain or temperature changes, tingling or burning sensations, sharp pains, or cramps. Some people with this condition experience amplified sensitivity to touch, muscle weakness, and loss of reflexes, especially in the ankles. Loss of balance and coordination, and severe foot issues such as ulcers, infections, and bone and joint pain can also be indicators of peripheral neuropathy.
Autonomic Neuropathy
The autonomic nervous system controls your heart, bladder, stomach, intestines, sex organs, and eyes. Diabetes can have an impact on nerves in these parts of the body. Bladder problems such as urinary tract infections, urinary retention, or incontinence can result from autonomic neuropathy. Other issues include constipation and uncontrolled diarrhea. People experience slow stomach-emptying, which can cause nausea, vomiting, bloating, and loss of appetite. Difficulty swallowing, increased or decreased sweating, problems controlling body temperature, and changes in how your eyes adjust from light to dark might all occur with this type of neuropathy. It can increase your heart rate while at rest. Sharp drops in blood pressure after standing can cause you to feel lightheaded. A person with autonomic neuropathy may also experience erectile dysfunction, vaginal dryness, and decreased sexual response.
Radiculoplexus Neuropathy
Radiculoplexus neuropathy impacts nerves in the thighs, hips, buttocks, and legs. These signs of neuropathy are common in people with type 2 diabetes and older adults. Symptoms tend to affect only one side of the body but may spread to the other. Eventually, this condition causes the thigh muscles to get weak and shrink. People may find it difficult to rise from a sitting position. Abdominal swelling can lead to unexpected weight loss.
Mononeuropathy
Mononeuropathy, or focal neuropathy, damages a particular nerve in the face, the middle of the body, or the leg. It usually occurs in older adults. Mononeuropathy often attacks suddenly and can cause extreme pain, though long-term issues are rare. The symptoms, which depend on which nerve is affected, generally go away without treatment over a few weeks or months. You may experience pain in the shin or foot, lower back, or pelvis. Also, the front of the thigh, chest, or abdomen can hurt. Mononeuropathy can also cause nerve problems in the face and eyes, which may lead to trouble focusing, double vision, and aching behind one eye. In some cases, individuals with mononeuropathy develop Bell’s palsy or paralysis on one side of the face.
Diagnosis of Neuropathy
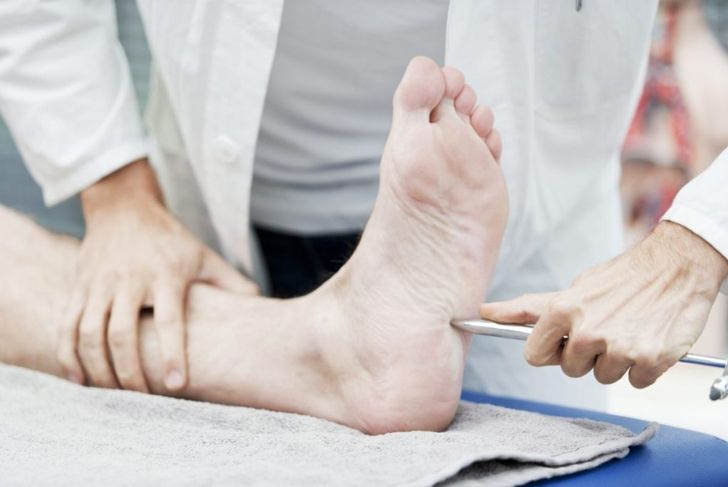
A doctor can generally diagnose neuropathy by carrying out a physical exam and carefully reviewing your symptoms and medical history. He or she will check your general muscle strength, tone, and tendon reflexes. Your sensitivity to touch and vibration might also be a factor. At each visit, you should have your feet examined for sores, cracked skin, and blisters, as well as bone and joint issues.
Additional Examinations
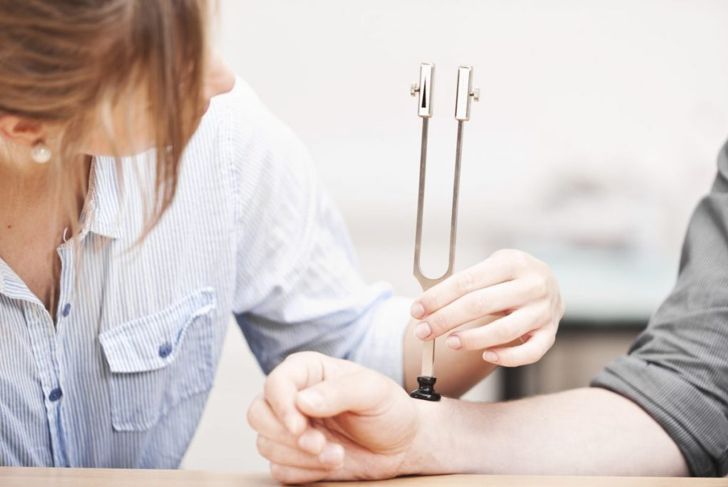
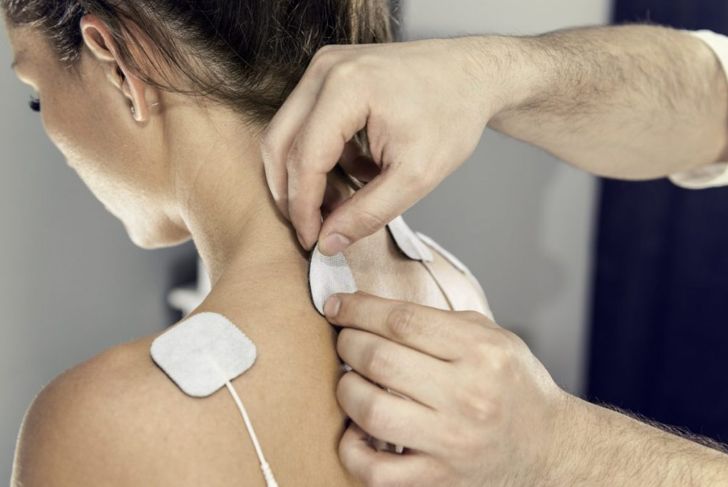
Along with your physical exam, the doctor may order tests such as a filament test, which involves brushing a nylon fiber over the skin to test your sensitivity to touch. A quantitative sensory test will determine how your nerves respond to vibration and changes in temperature. Nerve conduction studies measure how quickly the nerves in your arms and legs conduct electrical signals. You might also receive electromyography or an EMG. This test measures the electrical discharges produced in your muscles. Blood pressure tests and tests that determine sweat production may also be ordered.
Treatment for Neuropathy
Diabetic neuropathy, unfortunately, has no cure. Many different things can assist in making you feel better, but there is no known cure. The goals of treatment are to slow down the progression of the disease, relieve pain, manage the problems, and restore function.
Slowing Down Neuropathy
To delay nerve damage, always keep your blood sugar within your target range. Your doctor will determine what your target should be; this is different for each person and depends on many factors such as age and weight. Keep in mind your medical provider may adjust this target range as time goes on. Other ways to help slow or prevent the progression include controlling blood pressure and weight.
Pain Relief for Diabetic Neuropathy
There are many prescriptions available for diabetes-related nerve pain, but they don’t work for everyone and can have side effects. A doctor may prescribe an anti-seizure drug, which has the added benefit of reducing nerve pain. Unfortunately, these medications can cause drowsiness, dizziness, and swelling. Antidepressants can disturb the chemical processes in the brain that make you feel pain. The doctor may also prescribe a combination of these types of drugs and painkillers.
At-Home Relief of Diabetic Neuropathy
You can take in your lifestyle and try home remedies to relieve nerve pain. Eat a balanced diet that includes a variety of healthy foods like fruits, vegetables, and whole grains. Limit portion sizes to help achieve or maintain a healthy weight. Be active every day to keep your blood sugar under control and improves blood flow. These practices may not control pain on their own, but can help and could reduce the need for medication.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More