Vasovagal syncope is a fainting episode that can affect people of any age or gender and may be triggered by a host of factors. Luckily, there are no long-lasting effects from an episode of vasovagal syncope. Future episodes can be prevented by avoiding known triggers and recognizing the signs of an impending fainting spell, while medication can treat chronic cases.
What is It?
Vasovagal syncope is fainting that occurs when the body overreacts to a trigger. The common condition affects young adults and children most often but can happen to anyone at any age. Men and women experience vasovagal syncope equally. It is usually harmless, does not require treatment, and does not signal an underlying condition in the brain or heart.
Causes of Vasovagal Syncope
Vasovagal syncope occurs when the nervous system sends inappropriate signals through the body. Nerves help regulate blood pressure by constricting or dilating the vessels. Typically, the brain receives enough blood from this process, but when the nerves do not deliver the right signals, blood vessels dilate and the heart can slow down. Blood then pools in the legs, causing blood pressure to drop. The brain gets too little blood, and this results in a loss of consciousness.
Triggers
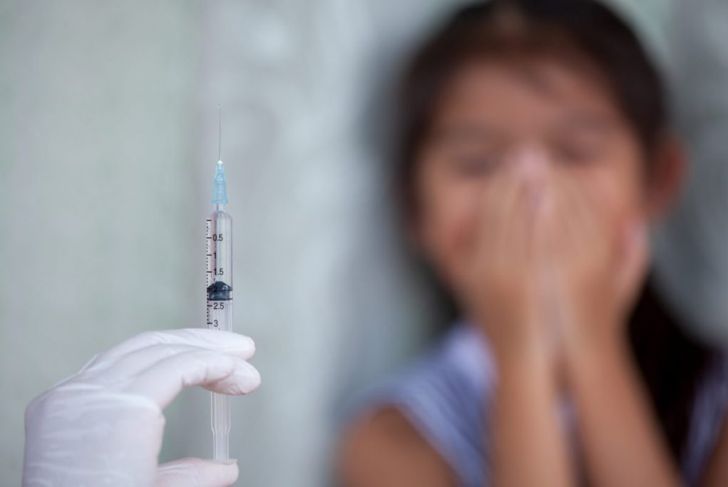
Several factors can trigger this reaction in the body, including excessive heat, intense pain, dehydration, coughing, swallowing, urinating, or bowel movements. Intense emotions, prolonged exercise, standing for a long time, or the sight of a needle or blood can also be triggers. Someone who has experienced fainting in the past should actively avoid their personal triggers.
Symptoms
Several symptoms may show up prior to a vasovagal syncope episode, including lightheadedness, pale skin, tunnel vision, and yawning. Other signs that can occur are nausea, hot flashes, blurred vision, and a cold, clammy sweat. People who witness someone experiencing vasovagal syncope may notice that they have dilated pupils or a slow, weak pulse.
Preventing Vasovagal Syncope
Avoiding triggers is the best way to prevent future fainting episodes. Some people who experience these episodes often can identify the preceding symptoms and take necessary measures such as lying down, which can prevent a fainting episode because it helps blood get to the brain, and ensures if the person does faint, he does not hurt him.
Recovery
When someone faints from vasovagal syncope, laying down restores the blood flow to the brain and the person should regain consciousness quickly. However, some people experience feelings of exhaustion or nausea after an episode. Most people experience vasovagal syncope once or twice in their lifetime, but others may have chronic fainting episodes that can occur for seemingly no reason.
Diagnosis
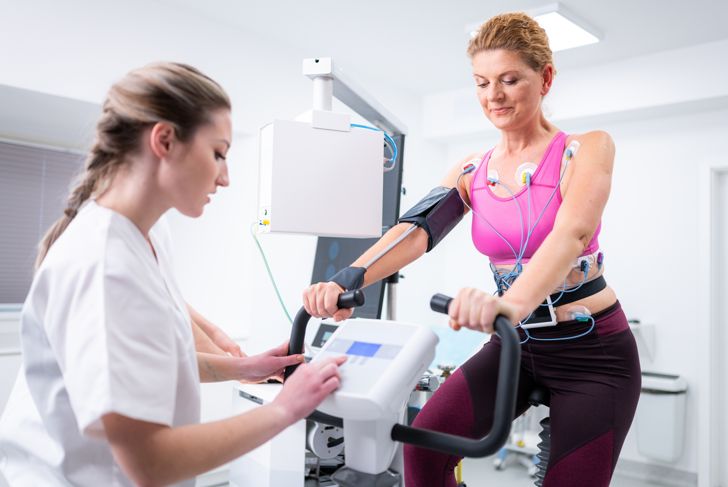
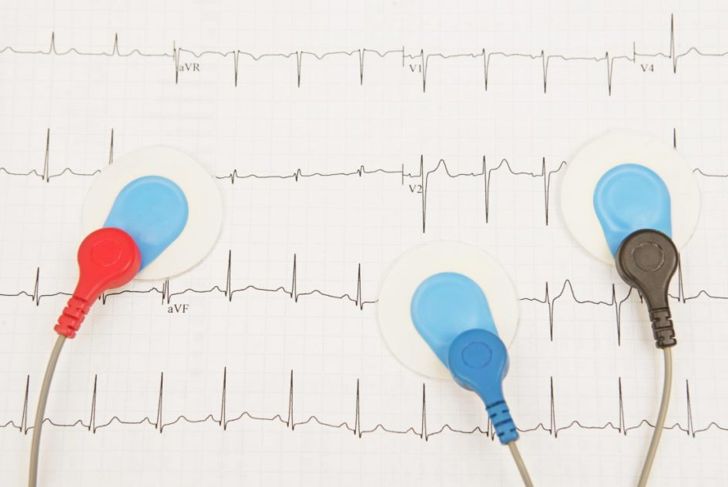
Diagnosing vasovagal syncope centers on ruling out other conditions, especially heart conditions that can disturb blood flow to the brain. Testing may include an electrocardiogram to detect an irregular heartbeat and other cardiac problems, an echocardiogram to view the structures of the heart, or a stress test to determine how the body reacts during exercise. Blood tests may rule out anemia and other issues that can lead to fainting.
Tilt Table Test
If everything appears normal after the first round of tests, the doctor may perform a tilt table test to monitor the body’s response to postural changes. The person lies flat on their back on a table that changes positions, tilting at various angles. Machines monitor heart rhythm and blood pressure throughout the test to see if they are affected by body positioning changes.
Treatment
Anyone who witnesses someone experiencing vasovagal syncope should try to help the person lay down with their legs elevated to help restore blood flow to the brain. People who have experienced vasovagal syncope should avoid triggers, stay hydrated, and wear compression stockings to prevent blood from pooling in the legs. They should also talk to their doctor about discontinuing any medications that lower blood pressure.
Medication
For people who have multiple episodes of vasovagal syncope, medication can help; they can increase blood pressue or moderate the nervous system response (using SSRIs). Corticosteroids increase sodium and, subsequently, fluid levels. These interventions are usually not recommended for people who experience rare or occasional fainting.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More