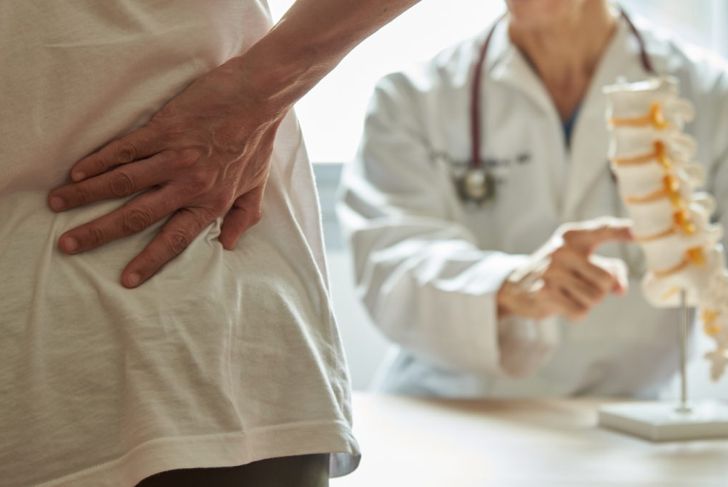
A bulging disc is a common condition of the spine. While a lot of people use the term interchangeably with a slipped disc or herniated disc, these conditions have unique identifying characteristics and defining traits. Depending on the severity, a bulging disc can be an asymptomatic normal sign of aging, or it can cause significant pain.
Bulging Disc
A bulging disc extends beyond the ridges of the endplate or ring apophyses — the edge of the disc, though this depends on how much of the disc is affected. When it affects less than 25 percent of the disc’s circumference, it is a protrusion. When it affects more than 25 percent, it is a bulge. Interestingly, neither of these is considered a herniation.
Annulus Fibrosus
The discs of the spine are rubbery pads that are about a quarter of an inch thick. They have a tough outer membrane called the annulus fibrosus, and a softer, flexible core — nucleus pulposus. The annulus fibrosus is made of rings of collagen that dehydrate and stiffen over time. A bulging disc affects only this membrane.
Degenerative
The deterioration that leads to bulging discs is usually age-related. Discs lose their elasticity and begin to bulge downwards. This can affect multiple discs and may lead to other spinal conditions, like lumbar stenosis. Bulging discs can occur at any point along the spine, but they are most common in the lumbar region.
Minor Bulging is Normal
Bulging discs are considered normal in some cases, particularly if they do not cause pain or interfere with the person’s quality of life. Asymptomatic people may have minor bulging, most often from the seventh lumbar vertebra to the first sacral vertebra in the lower back. This can result from osteoporosis, trauma, or other spinal deformities.
Not a Specific Diagnosis
A bulging disc is not a specific diagnosis. Rather, it is an observation made from an image of the spine and be attributed to multiple things. It may not even indicate a true pathological change in the body and, sometimes, people with bulging discs do not even know they have them until getting a scan for some other reason.
Symptoms
At some point, almost everyone has a bulging disc somewhere in their spine. Though they rarely cause symptoms, if the disc is weak enough and the pressure grows, they can increase in severity, eventually getting larger and becoming a protruding disc. If the bulge is pushing against the nerves, it can cause tingling, weakness, or numbness.
Imaging
Most bulging discs affect the lumbar spine, and multiple imaging techniques can evaluate it, depending on the pathology. The doctor will usually do an X-ray first, to identify the reason for back pain. CT scans are also useful to evaluate trauma and complex fractures, and MRIs provide in-depth information about the spinal cord, meninges, and nerve roots.
Treatment
When a bulging disc is symptomatic, there are multiple treatment options available. Over-the-counter NSAIDs are effective against mild pain, but the doctor may recommend steroid injections to relieve significant nerve pain. If the bulging disc progresses to the point of lumbar stenosis, a patient may require spinal decompression surgery.
Herniated Disc
The main difference between a bulging disc and a herniated disc is the part of the disc that is affected. A bulging disc involves only the annulus fibrosis, but a herniated disc may affect the annulus fibrosis, nucleus pulposus, cartilage, or the apophyseal bone. A herniated disc must-have material displaced from its normal location. It only occurs when there is a defect or other abnormality.
Degenerative Disc
A degenerative disc is another term used interchangeably with a bulging disc, though they are not the same. This term includes both pathologic changes and changes of normal aging. Disc degeneration is graded based on observations from CT scans of the interior of the disc and marrow changes seen on an MRI and may or may not include a bulging disc.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More