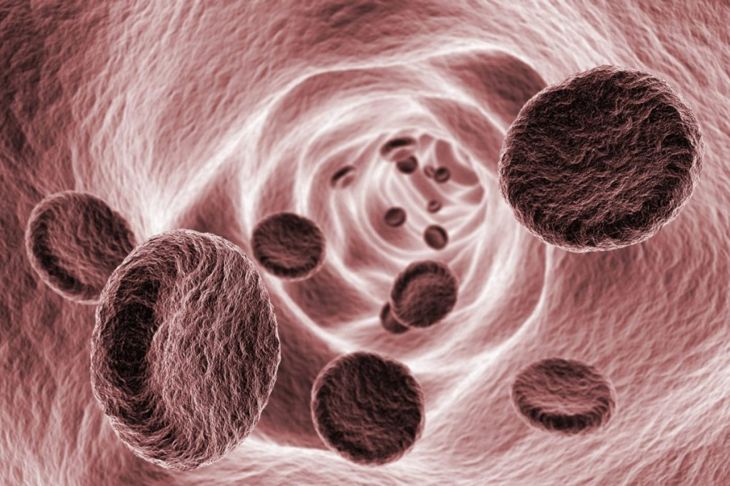
Peripheral vascular disease (PVD) is a common circulation disorder that occurs when the arteries or veins narrow and restricts blood flow. About 8.5 million people in the U.S. have this condition. PVD most commonly affects the legs and feet, but the disease can restrict the flow of blood anywhere outside of the heart, including the arms or other organs. When oxygen-rich blood cannot reach all of the body’s tissues, life-threatening complications can occur.
Causes of Peripheral Vascular Disease
The main culprit behind the narrowing of the peripheral arteries is a buildup of plaque from atherosclerosis. But blood clots can also form inside an artery’s wall and restrict or block the flow of oxygen and nutrients. People can develop PVD as a result of an injury to a limb or a congenital disability that causes irregular muscle or ligament anatomy. Inflammation of blood vessels from infection can also be responsible for PVD, and so can exposure to radiation, such as the type used in cancer treatment. It can damage blood vessels and contribute to the development of PVD.
Risk Factors
Some factors raise the chances of developing peripheral vascular disease. Being over age 50, having a personal or family history of heart disease or stroke, or being male or postmenopausal raises the risk. Other factors that increase the odds of getting PVD include cigarette smoking, diabetes, elevated LDL cholesterol, high blood triglycerides, low HDL cholesterol, high blood pressure, and obesity. Physical inactivity also contributes.
Symptoms
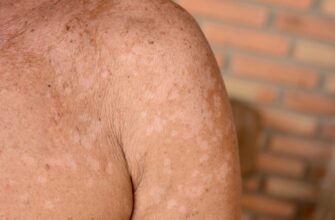
One of the first symptoms of PVD that affects the leg is muscle cramping or fatigue during exercise, with the calf being a common location of discomfort. The pain typically goes away with rest. Other signs include numbness or weakness in a limb, sores that won’t heal, and skin that looks shiny. People with more advanced PVD may feel pain in their affected extremities, like the toes or feet, even at rest. About half of people don’t notice any symptoms, which is why anyone with risk factors for the disease should talk to their doctor about screening.
Complications
When arteries have blockages, and sufficient blood can’t reach the limbs, brain, or organs, those under-supplied areas become damaged, and infection or tissue death, called gangrene, can occur. A person with PVD may develop sores that don’t heal, and their risk of stroke is significantly higher than for those who don’t have PVD. They could even lose a limb as a result. People who smoke tobacco products or have diabetes have the greatest risk of developing complications because both can impair blood flow.
Diagnosis
A simple test for lower-extremity PVD is a blood pressure reading that a medical professional takes at the ankle and compares to blood pressure in the arm. To detect where there is a narrowing of the arteries, a CT or MRI scan can capture an angiogram. Doctors use a range of non-invasive tests to identify and assess PVD, including ultrasounds and treadmill exercise tests.
Treatment
Treatment for PVD usually focuses on lifestyle changes, such as quitting smoking, beginning an exercise program, and taking medications. It is also important to manage contributing conditions, like diabetes and high cholesterol. Surgical procedures can treat severe cases by removing blockages. In many cases, people with PVD can slow down the disease or even reverse its symptoms, particularly when it is caught early.
Prevention
Much like treating PVD, preventing the disease is mostly about managing risk factors and following a healthy lifestyle as much as possible. Not smoking, limiting saturated fat and cholesterol intake, and maintaining a healthy weight can all help. Daily exercise, with a doctor’s approval, is also beneficial because it improves circulation by creating new blood vessels.
Exercise
Studies show that walking helps reduce the symptoms of PVD that affect the legs. In one study, a six-month walking program showed advantages over surgery. Experts recommend that people with PVD participate in supervised exercise whenever possible, rather than going it alone. Make sure to stretch and warm up, then alternate walking and resting, building up to 50-minute walks at least three times a week.
Stress
Reducing stress is an important component of preventing and managing PVD. One study demonstrated a small but consistent link between work-related stress and hospitalization due to peripheral vascular disease. The reason for that connection is unclear, but the authors suggest that stress-related inflammation may play a role.
When to Seek Help
It is always best to detect and treat PVD as early as possible. People should see a doctor if they have symptoms like leg pain that goes away with rest or wounds that do not heal. Also, many symptoms of PVD are signs of other conditions, as well, so it is always wise to get a check-up. Anyone with known risk factors should request a screening for peripheral vascular disease.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More