When four patients died suddenly from cardiac events in 1992, Drs Josep and Pedro Brugada saw something on the ECGs, that was inexplicable. After identifying four more patients, they published these findings and opened up a new area in medicine on sudden, unexplained cardiac death. Brugada syndrome is a disease that increases the risk of fatal abnormal heart rhythms. After this initial discovery, it would take another six years for their brother, Ramon Brugada, to find a potential genetic cause for this disorder, which affects between 1 and 30 in every 10,000 people.
What is Brugada Syndrome?
Brugada Syndrome causes serious, abnormal heart rhythms, such as ventricular fibrillation, where the heart quivers instead of pumps, or polymorphic ventricular tachycardia, fast heart rate caused by improper electrical activity. Both of those conditions put individuals at risk for sudden cardiac death. The signs and symptoms of Brugada are vasovagal syncope, a sudden drop in blood pressure that causes blackouts or an untreated heart rhythm that causes sudden death.
Faulty Communication
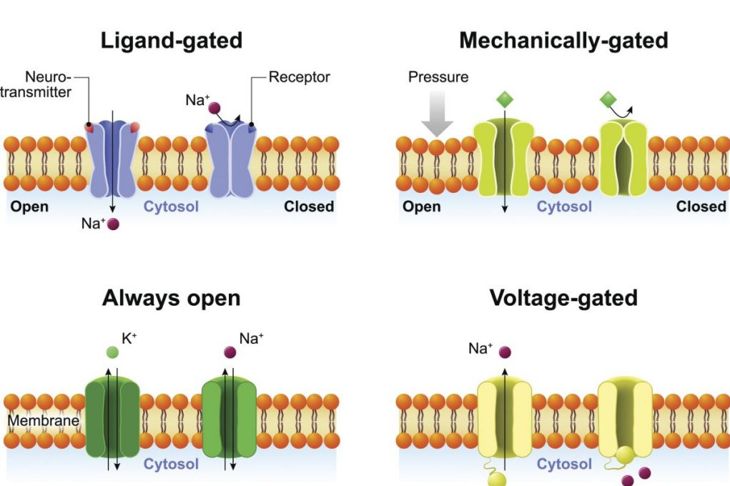
Cells communicate via electrical signals transmitted by substances called electrolytes. This communication network is disrupted, specifically in the cardiac sodium channel. Sodium channels deal with action potentials, meaning that they activate certain intracellular processes. In the heart, they are in charge of the rest, active, and inactive states. Misfiring of or miscommunication between these channels leads to irregular functioning.
Role of Genetics
The primary cause of less than 40 percent of clinical Brugada cases is 250 genetic mutations happening over 18 genes. This disease is an autosomal dominant mutation that only needs one parent to carry the mutations to give the child a 50-percent chance of inheriting the disorder. Chromosome 3 is the primary gene that’s scrutinized, because it produces a protein that helps sodium atoms move through the channel and into the heart muscle cells. Reduced sodium leads to arrhythmia.
Other Causes Of Brugada
While genetics does play a significant role in Brugada, there are other potential causes of this heart rhythm disorder. Having an hard-to-spot structural heart abnormality is one non-genetic cause. Unfortunately, the only time this may be detected is during a life-threatening episode. Another cause is having an imbalance of electrolytes, such as potassium, calcium, or sodium, that assist in electrical signal transmission and heart functionality.
Diagnosing Brugada
Diagnosis usually happens in two phases. First, doctors orders a 12-lead ECG to record the heart’s electrical activity. Since the disorder is a sodium channelopathy, a disease that causes the disturbed function of the sodium ion channels, they may prescribe medication that will draw out the Brugada pattern, so that it’s visible on the print-out. Based on those results, they may order lab tests and genetic testing to further confirm the diagnosis. However, if the ECG was inconclusive, an EP test, where catheters are placed inside the heart to get a more in-depth picture of its activity, could be ordered.
Who’s at Risk?
Brugada affects men and women but doesn’t really manifest until after 40. However, studies show that men are five to eight times more likely to have the disorder, and it’s seen more in individuals in Southeast Asia and Japan. While Brugada is rarely diagnosed in younger people and children, research suggests that it can present in two ways. SUNDS, sudden unexpected nocturnal death syndrome, is a condition that causes cardiac arrest in young people of the Southeast Asian population, while they sleep. It may also presents as SIDS, sudden infant death syndrome, in children one year or younger.
Drug-induced Brugada Syndrome
According to research, there are certain types of drugs that can induce the disorder. Tricyclic antidepressants that are taken over the prescribed levels can trigger antiarrhythmic action. Certain anesthetics taken at high doses may reveal Brugada, but when it comes to antihistamines, the study showed that Brugada was induced with first-generation antihistamines that typically cause sedation. Finally, researchers state that cocaine has strong sodium channel blocking effects, which can provoke a fatal cardiac event.
Fever-induced Brugada Syndrome
Diagnosing Brugada is already challenging. Studies show that only every third ECG showed a Brugada pattern and every third was considered normal. But in situations of fever, those who may have undiagnosed Brugada are more likely to exhibit symptoms. One reason is during sickness, the sodium channel that’s already dysfunctional, will be further exacerbated and is more likely to show up on the graph. Secondly, having a fever can precipitate arrhythmias. This form of the condition is still being studied, so scientists aren’t sure how rare or common it is.
Managing Brugada Syndrome: Lifestyle Changes and Medications
There is no cure for Brugada Syndrome; there’s only management for those who know that they have it. While this type of arrhythmia doesn’t usually show up during physical activity, doctors recommend avoiding strenuous exercise. Avoiding excessive alcohol consumption is another recommendation along with not taking certain medications, especially when dealing with fevers. There are some prescribed antiarrhythmic medications that are effective in handling electrical storms that pop up in the heart.
Using an ICD
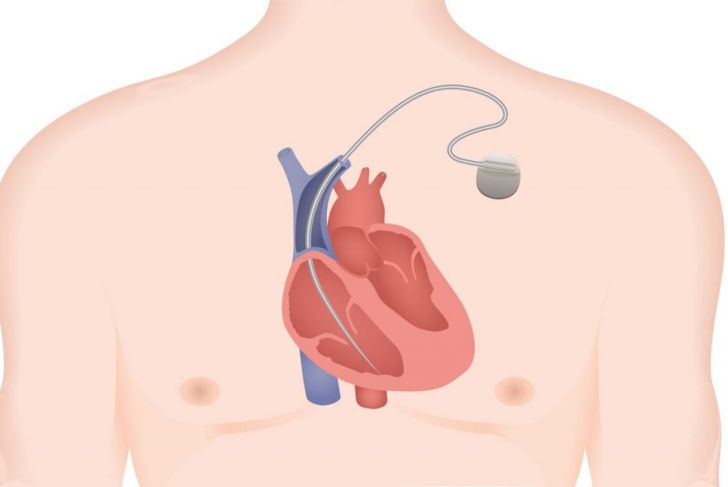
An implantable cardiac defibrillator, ICD, is a low-risk, effective procedure that monitors the heart’s rhythm and gives it an electrical shock, so that it falls back into a normal rhythm. It can also act as a pacemaker should the heart get too slow, which can happen to those with Brugada. As effective as these devices are, they can be costly and unavailable in certain countries. That’s why they are only recommended for those with a high risk of sudden cardiac death.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More