Anaplasmosis comes from parasites, specifically ticks that generally target ruminants such as cattle, deer, goats, and sheep. Though it is rare, these ticks may also latch onto dogs and humans and directly transmit anaplasmosis. Symptoms tend to vary depending on the age and general health of the infected animal or person.
Transmission
Anaplasmosis results from infections of the bacteria Anaplasma and its many variations. Most human cases of anaplasmosis are due to Anaplasma phagocytophilum. Ticks tend to receive the disease by feeding on already-infected animals, though some females transmit it through their eggs. Most people contract the disease via a tick bite, though it is possible for a person to contract the disease without being bitten by a tick. In some cases, anaplasmosis is asymptomatic, and a person may have the disease and not be aware of it. If this person donates blood, recipients may contract anaplasmosis.
History of Anaplasmosis in Humans
The first case of anaplasmosis in a human occurred in 1990. A patient in Wisconsin developed a feverish disease after a tick bite. Just two weeks later, the patient died. In 1994, experts identified human granulocytic anaplasmosis after years of research. The disease is almost indistinguishable from other tick-borne diseases such as Lyme disease or human monocytic ehrlichiosis. From 1994 to 2010, the rate of infection for human granulocytic anaplasmosis has increased significantly. Prior to 2000, there were fewer than 300 cases each year. From 2009 to 2010, there was a 52 percent increase in cases.
Responsible Parasites
Up to 17 tick species are capable of transmitting anaplasmosis. In humans, the Ixodes genus of ticks is usually responsible. These hard-bodied ticks include the western black-legged tick in the western United States or the Tasmanian paralysis tick in Australia. In the United States, the disease appears most commonly in the Northeastern and upper Midwestern states. One of the most common carriers of anaplasmosis bacteria is the white-footed mouse. Though other animals can carry the bacteria, they are usually infected with strains that do not cause human granulocytic anaplasmosis.
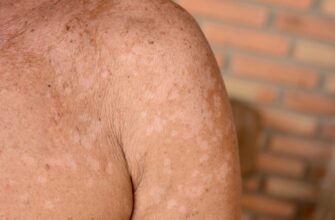
Symptoms
Usually, the incubation period following a tick bite is between one and two weeks. Most tick bites are painless, and few people realize they were bitten. Though asymptomatic infection is possible, early symptoms include fever, chills, headaches, muscle aches, and stomach issues such as vomiting, diarrhea, and nausea. If a person does not receive treatment or if they have other medical conditions, anaplasmosis may lead to serious illness, with symptoms such as respiratory failure, organ failure, bleeding issues, and even death. Older individuals and people with weaker immune systems are particularly at risk for life-threatening complications.
Prevention
Currently, there is no vaccine to protect against anaplasmosis. Individuals who spend time outdoors should be aware of the types of ticks in their area. Most ticks thrive in grassy and wooded locations and on animals. They are generally active in the warmer months between April and September. Many chemical products can protect against ticks when sprayed on clothing, and hikers should take care to avoid tall grass where possible. Always examine gear and pets following an outdoor venture and shower soon after being outdoors.
Anaplasmosis in Dogs
When it comes to tick bites and infections, many people worry about their pets’ health, particularly dogs who accompany their owners on walks and hikes. Generally, dogs are not as at risk of anaplasmosis as other animals. However, the brown dog tick can carry the Anaplasma platys bacteria, which can lead to a weaker form of anaplasmosis. Dogs who are lethargic or lacking an appetite, coughing, having difficulty breathing, or experiencing stomach issues could be infected. Symptoms usually do not last longer than a week. It is possible for anaplasmosis to lead to other diseases such as cyclic thrombocytopenia, which can cause nosebleeds and bruises. Veterinarians will treat the disease over several weeks, and most dogs respond excellently to treatment. There are no recorded cases of the death of a dog resulting from anaplasmosis.
Pet-to-Human Transmission
Some diseases that affect pets can eventually infect owners. Though anaplasmosis has the potential to infect humans, direct transmission is unlikely. Currently, there are no documented cases of direct transmission from animal to animal or animal to human. However, it is possible that an infected tick could fall off of a pet and then bite a human, thereby transmitting anaplasmosis to both.
Removing Ticks
Individuals who notice ticks on themselves or their pets should take care removing the parasites to avoid transmission of any diseases. A person should never grab or squeeze a tick’s body, particularly if it appears bloated. Instead, gradual traction on the tick’s head with small forceps will dislodge the parasite without risking transmission. Often-recommended methods such as matches, petroleum jelly, and other irritants are not effective methods of tick removal and may increase the risk of disease transmission. After removing the tick, rubbing alcohol can reduce the chance of infection.
Diagnosis
Doctors use many tests to diagnose human granulocytic anaplasmosis. The disease affects white blood cells called neutrophils, and examination of these cells can reveal the infection. Alternatively, doctors can use polymerase chain reaction testing of a blood sample. Though this is not widely available, it is the most effective method of diagnosing many diseases. Essentially, the test multiplies pieces of bacteria and then chemically detects the presence of the bacteria. It is often difficult to diagnose anaplasmosis, and doctors may refer patients to infectious disease specialists.
Treatment
Physicians will often begin treatment for anaplasmosis before confirming the presence of the disease because the treatments are not harmful and every moment matters in preventing advancement. Typically, treatment begins with antibiotic medications. These may be self-administered at home, or the individual may need to come to the hospital. People with severe cases may spend time in an intensive care unit.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More