Facet arthropathy or facet arthritis is a disease of the facet joints in the spine. One of the most common causes of this condition is osteoarthritis, though there are other contributing factors. Symptoms of facet arthropathy can be exacerbated by other issues, such as spinal stenosis or degenerative disc disease. While pain is the most common symptom, additional issues may develop depending on where along the spine the problem lies. The location can make a big difference in how the person experiences the pain.
Osteoarthritis
Osteoarthritis occurs when the cartilage that cushions the ends of the bones begins to wear down. The most prevalent form of arthritis, osteoarthritis affects millions of people all over the world. The hips, knees, hands, and spine are the most commonly affected joints. When osteoarthritis occurs in the spine, it leads to facet arthropathy. This damage can usually be managed effectively but cannot be reversed.
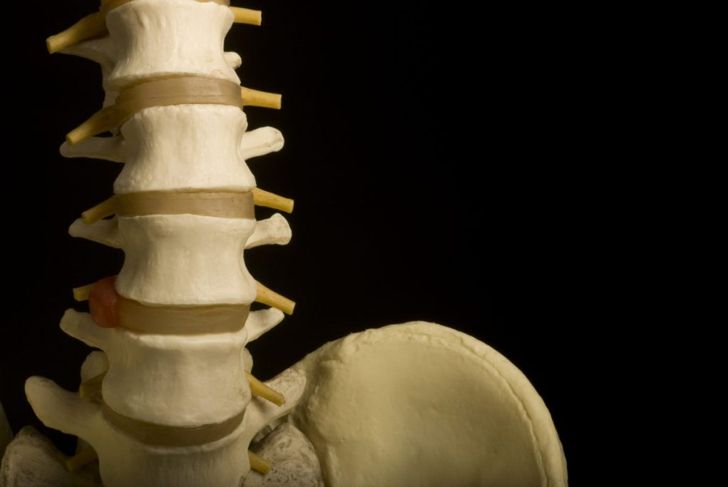
Facets
The facet joints connect the bones in the spine. Nerves from the spinal cord pass through the facets and out to the limbs and other parts of the body. The joints facilitate movement, too, allowing the body to turn from side to side and bend while keeping the back from moving too far. The cartilage helps the bones move smoothly against each other, which is why someone with facet arthropathy experiences so much pain.
Disease Process
The severity of symptoms depends on the severity of the disease. Generally, osteoarthritis presents with pain during or after periods of movement. If the cartilage continues to wear down, the pain progresses. Swelling and stiffness can also occur. Eventually, loss of flexibility progresses to where the person may feel a grating sensation between the joints as more and more cartilage wears away. Burn spurs can also develop around the affected joints.
General Symptoms
As mentioned, back pain is the most common symptom of facet arthropathy. This pain is distinctive, as it is felt deep within the back, gets worse when standing, and is alleviated by laying down. Intermittent low back pain is usually the first sign that something is wrong. Other symptoms include curvature of the spine, a stooped posture, and hip deformities. These symptoms do not progress at a steady pace and can come and go, sometimes permanently.
Cervical Region
Some symptoms of arthropathy depend on where along the spine the damage is located. If it occurs in the cervical region, pain is typically localized at the neck, but it can also radiate to the middle of the shoulder blades or shoulder girdle. If the facet arthropathy occurs high enough in the cervical region, it can also cause headaches.
Lumbar Region
Facet arthropathy in the lumbar region can cause referred pain in the buttock and thigh. This pain is not limited to the back of the legs and can radiate around the whole thigh to the front of the body, though it usually stops at the knee. Pain at or below the knee is possible but rare.
Cervical Risk Factors
Risk factors for cervical facet arthropathy differ from those of lumbar arthropathy slightly. Age is one of the most common risk factors for cervical facet arthropathy and its progression. Having a high body mass index (BMI) slightly increases the risk for both men and women, though gender itself does not seem to be a factor.
Lumbar Risk Factors
Age is also a factor in lumbar facet arthropathy. Women are more likely to develop it than men, and it is more prevalent in Caucasians than African Americans. Having a high BMI is a more significant risk factor for lumbar facet arthropathy than for cervical; this factor makes someone three to five times more likely to experience the lumbar form.
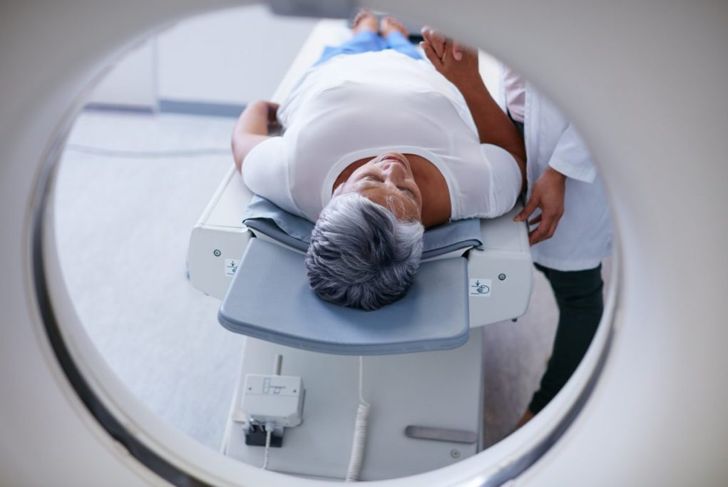
Diagnosis
Diagnosis of facet arthropathy can be difficult because there are not any definitive tests. Physical exams do not usually provide much information, either. MRIs and X-rays may show the spaces between facets narrowing or slipping or show edema around the joint. If the doctor suspects back pain is caused by facet arthropathy, they should encourage very explicit descriptions of their patient’s symptoms.
Treatment
Surgery is not typically recommended as a treatment for facet arthropathy, though in severe cases, spinal fusion or disc replacement may be necessary. Generally, treatment consists of physical therapy and anti-inflammatory medication. If applicable, the person will also be encouraged to lose weight to reduce the amount of pressure put on the spine.

 Home
Home Health
Health Diet & Nutrition
Diet & Nutrition Living Well
Living Well More
More